1. SVC Syndrome (Superior Vena Cava Syndrome)
① Definition of SVC Syndrome
Superior Vena Cava (SVC) Syndrome refers to a clinical condition caused by any obstruction of blood flow through the SVC.
- Malignant Obstruction:
Direct tumor invasion of the SVC or external compression due to adjacent pathological processes involving the right lung, lymph nodes, and other mediastinal structures can lead to venous congestion and thrombosis. - External Compression & Thrombosis:
In some cases, external compression and thrombosis coexist.
② Pathophysiology
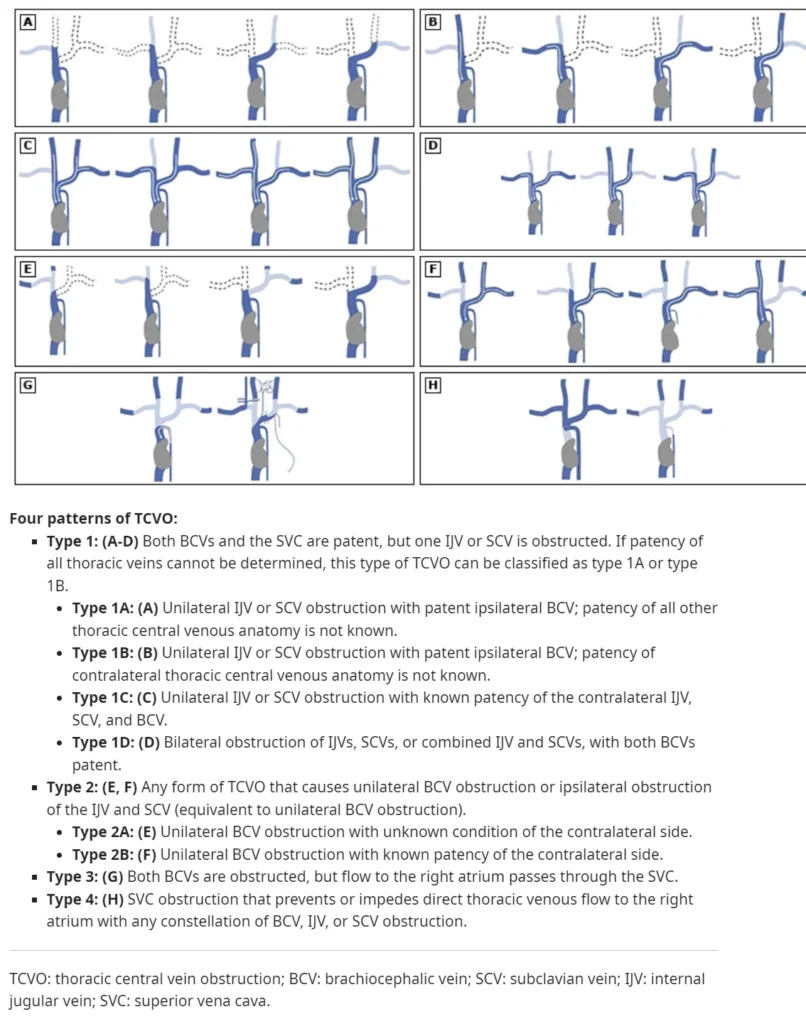
SVC obstruction is classified as a type IV central venous obstruction related to malignancy.
- Primary Mechanisms:
Extrinsic compression of the SVC by a primary tumor or mediastinal lymphadenopathy, or direct tumor invasion of the SVC. - Collateral Circulation Formation:
When blood flow in the SVC is obstructed, collateral veins form alternative pathways for venous return to the right atrium.- These collateral veins develop in the azygos system, internal mammary veins, lateral thoracic veins, paravertebral veins, and esophageal venous plexus.
- Collateral circulation expands over weeks; however, even with well-developed collateral pathways, central venous pressure (CVP) continues to rise, leading to the characteristic signs and symptoms of SVC Syndrome.
③ Malignancies Associated with SVC Syndrome
- Intrathoracic Malignancies: Account for 60–85% of SVC Syndrome cases.
- Non-Small Cell Lung Cancer (NSCLC): The most common malignant cause, responsible for ~50% of cases.
- Small Cell Lung Cancer (SCLC): Accounts for 25–35% of cases.
- Although less common than NSCLC, SVC Syndrome occurs in ~10% of SCLC cases at presentation due to rapid tumor growth in the central airways.
- Lymphoma: SVC Syndrome occurs in 2–4% of non-Hodgkin lymphoma (NHL) cases.
2. Clinical Presentation and Diagnosis
① Symptoms & Signs of Central Venous Obstruction
Patients may present with edema, chest pain, respiratory symptoms, and neurological deficits.
- Common Symptoms:
- Facial or neck swelling
- Dyspnea
- Sensation of facial fullness or head congestion, which worsens when leaning forward, lying down, or raising the arms
- Edema-related Complications:
- Narrowing of the nasal and laryngeal lumen, potentially impairing laryngeal and pharyngeal function
- Symptoms may include dyspnea, stridor, cough, hoarseness, and dysphagia
- Cerebral edema may cause headache, confusion, visual disturbances, or auditory impairment
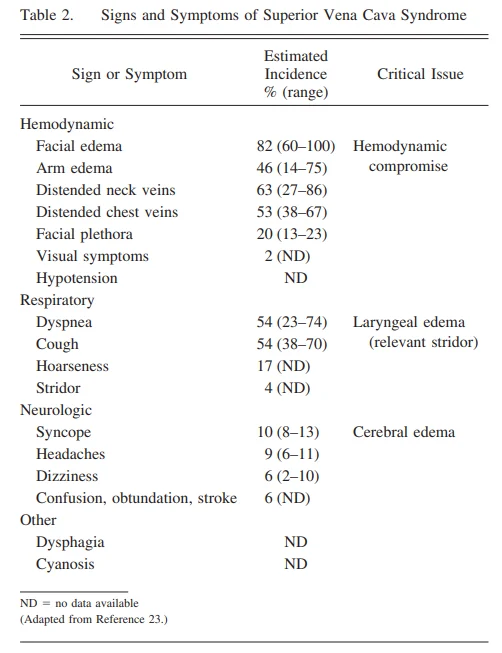

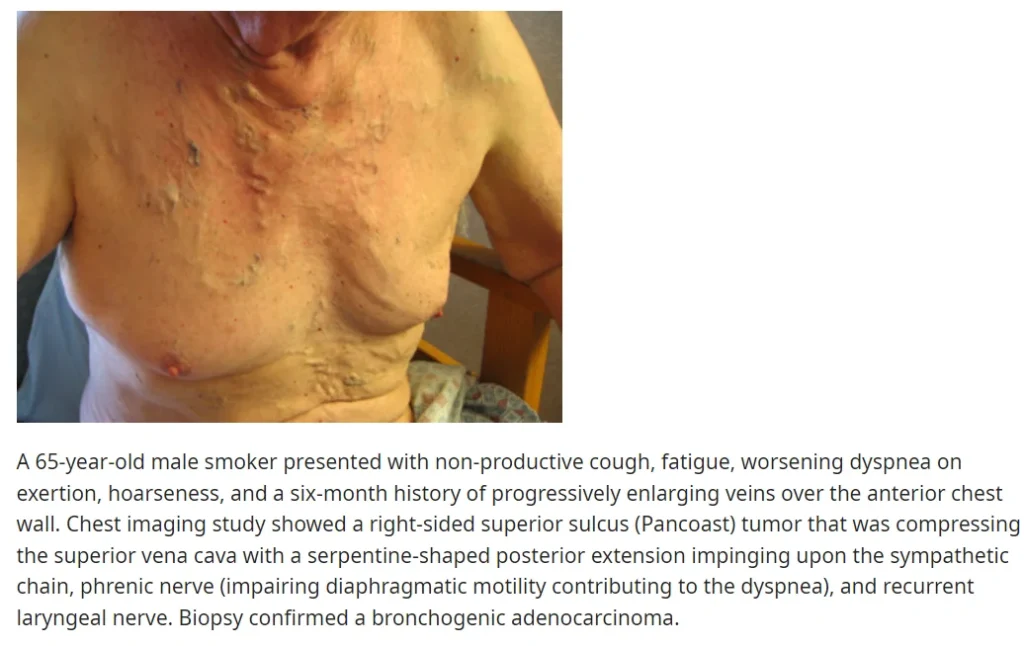
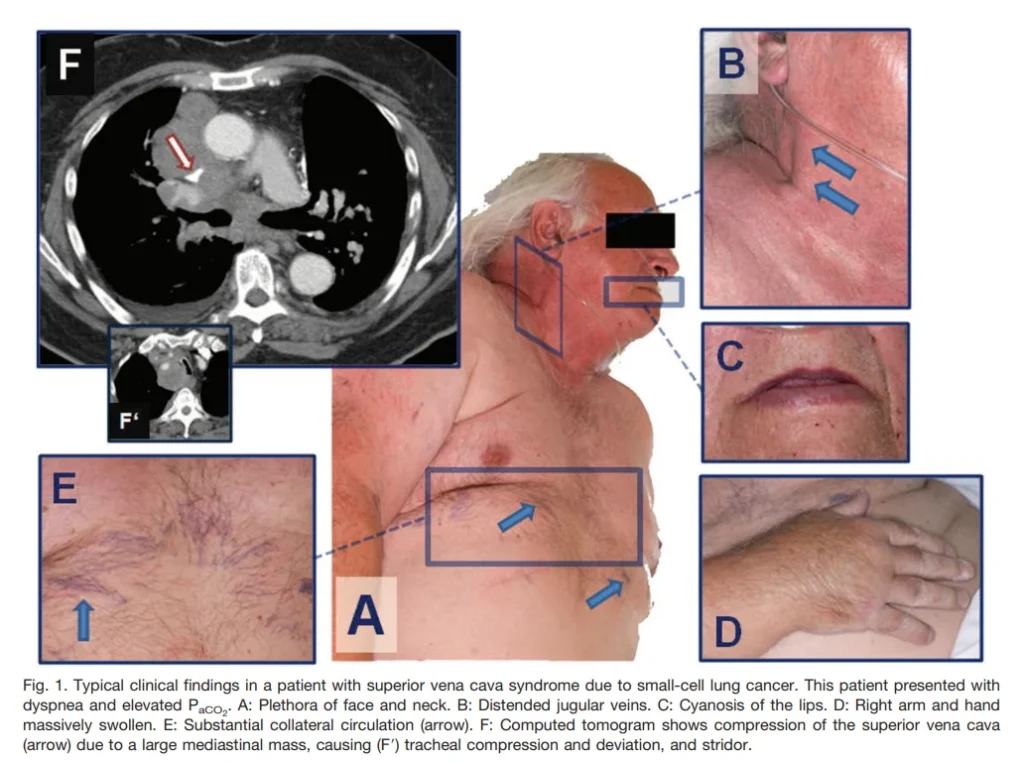
② Physical Examination
- Prominent venous distension in the neck and anterior chest wall may be observed.
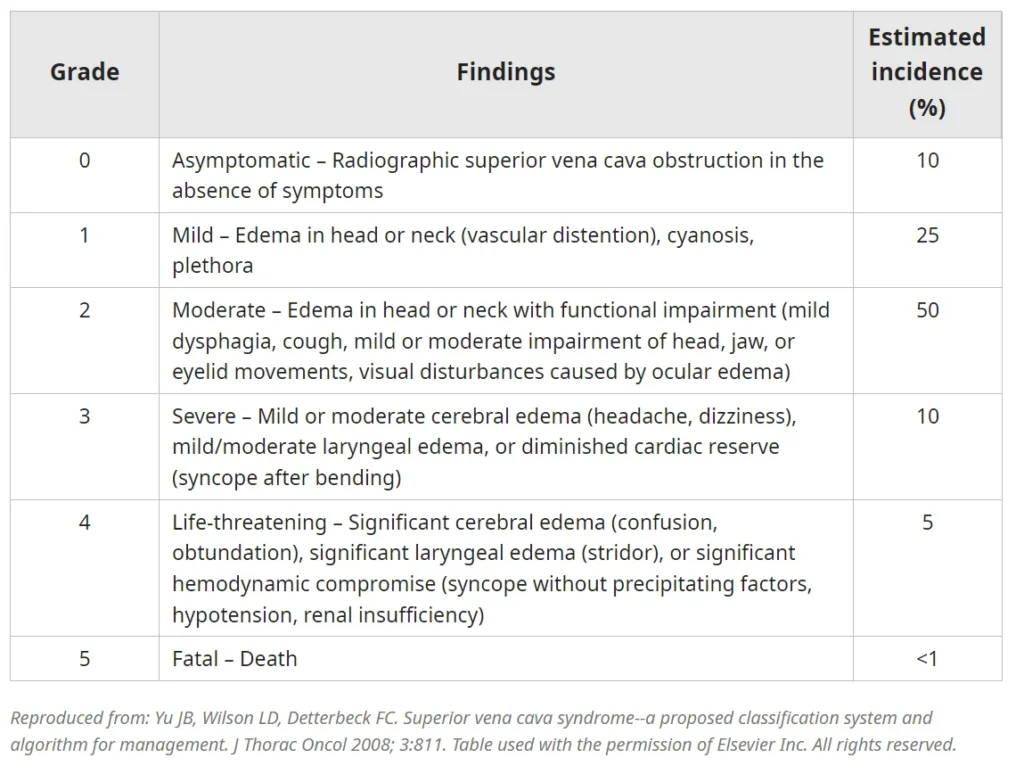
③ Severity Classification
- Patients are classified based on the severity of symptoms and clinical findings.
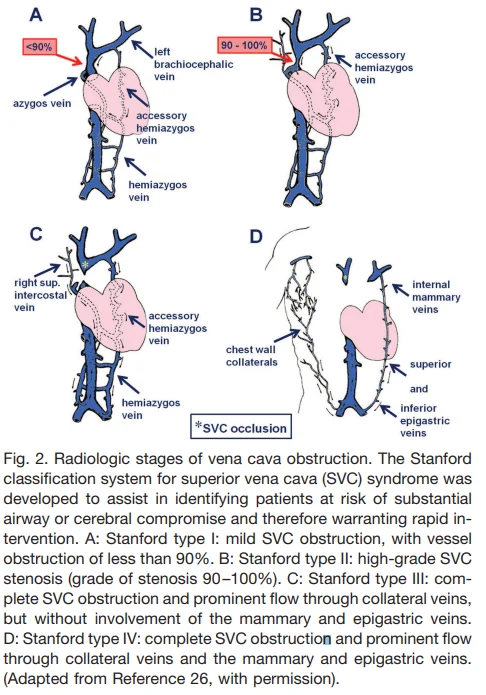
④ Diagnosis
- Clinical Diagnosis:
- Based on characteristic symptoms and signs of central venous obstruction.
- Imaging is required for confirmation.
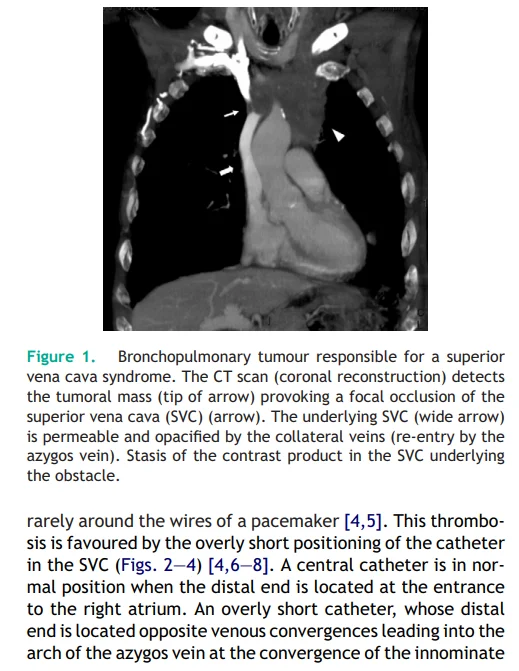
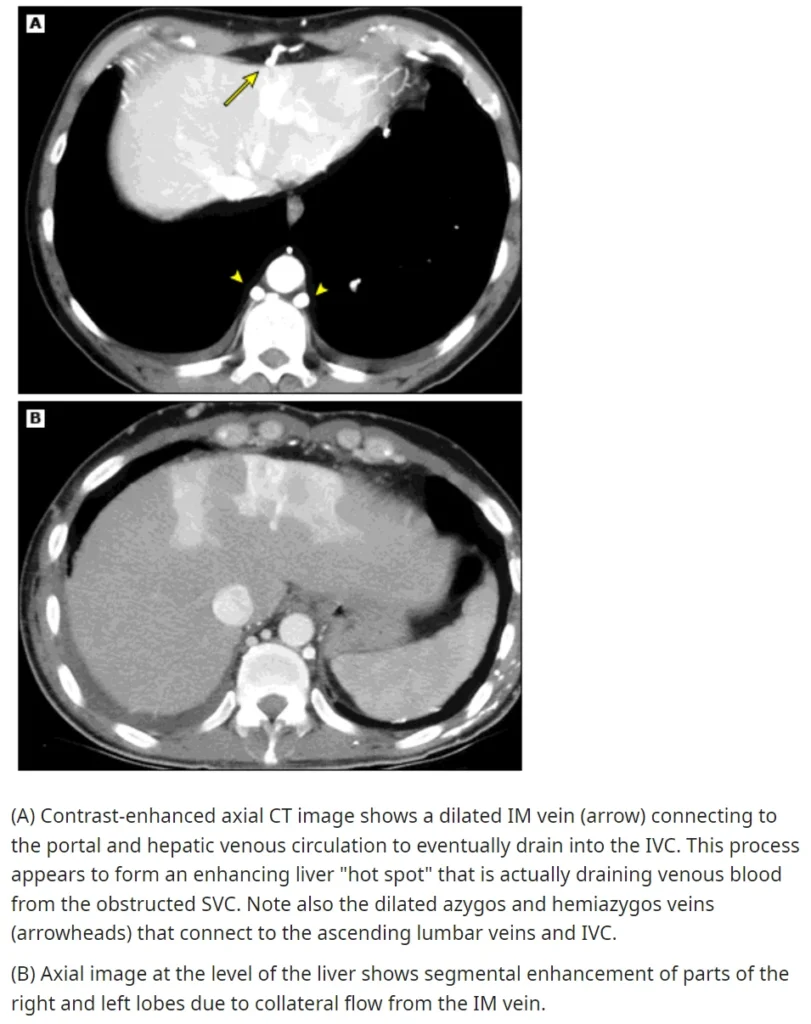
i) For Grade 3–4 Patients
- Contrast-Enhanced CT (CECT):
- Sensitivity: 96–98%, Specificity: 97–99%.
- The presence of collateral vessels on CECT is a strong indicator of SVC Syndrome (specificity: 96%, sensitivity: 92%).
- Helps determine the site, extent, and level of venous obstruction, which is crucial for planning endovascular intervention.
- Cross-sectional imaging provides insights into the underlying cause of obstruction.
- Alternative Imaging:
- MR Venography may be used when CT is contraindicated.
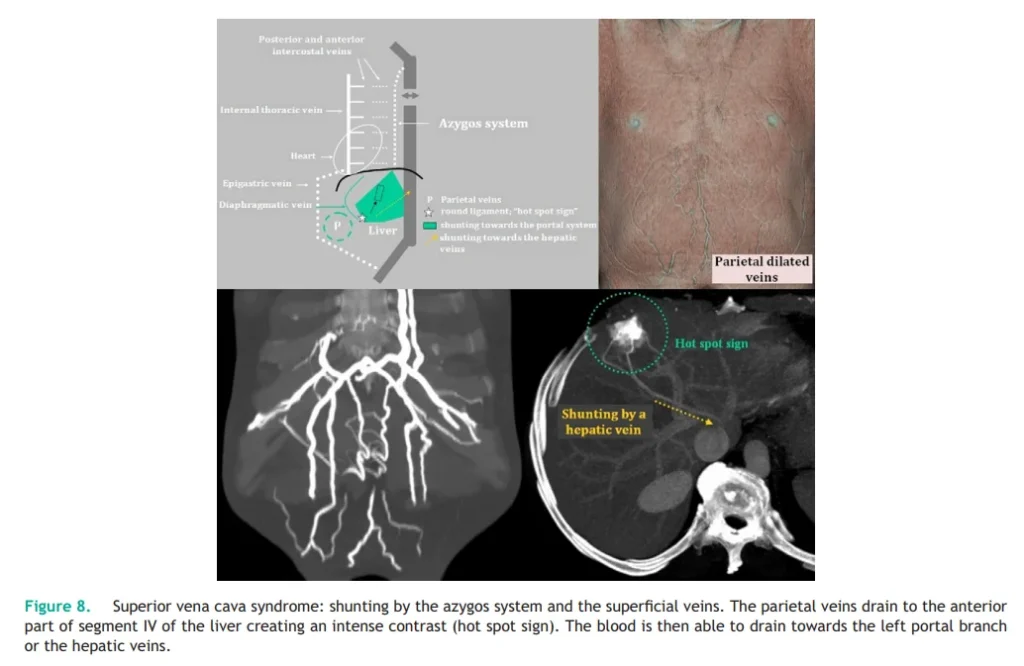
ii) For Grade 1–2 Patients
- Duplex Ultrasound:
- Useful for ruling out thrombosis in mild cases.
3. Treatment of SVC Syndrome
① Initial Management Goals
- Relieve symptoms & treat the underlying cause.
- Emergency Radiation Therapy (RT):
- No longer considered necessary for most patients.
- Current Guidelines:
- Emphasize accurate histologic diagnosis before initiating treatment.
- Highlight the importance of endovascular intervention (e.g., stent placement) for severe cases.
- Patients with severe airway obstruction due to central airway compression or laryngeal edema, or those with cerebral edema presenting with altered mental status:
- Require immediate airway stabilization (securing the airway, respiratory support, circulatory support).
- Urgent endovascular intervention (e.g., thrombectomy, stent placement) should be performed promptly.
- Emergency transfer to a facility with vascular interventional resources may be necessary.
② Management of Life-Threatening Symptoms
- Patients presenting with stridor, respiratory distress, or neurological impairment:
- Urgent endovascular intervention is preferred over initial RT.
- Patients with thrombosis:
- Anticoagulation is required unless contraindicated due to bleeding risk.
- Recommended anticoagulation therapy (Grade 2C):
- Dual antiplatelet therapy for 2–3 months:
- Clopidogrel monotherapy or a combination of clopidogrel and aspirin
- For malignancy-associated hypercoagulability:
- Low-molecular-weight heparin (e.g., enoxaparin) or direct oral anticoagulants (DOACs, e.g., apixaban) is preferred over clopidogrel.
- Dual antiplatelet therapy for 2–3 months:
③ Management of Non-Life-Threatening Cases
- Treatment varies depending on tumor histology and symptom severity.
- Endovascular Stenting:
- Restores venous drainage and provides rapid, sustained symptom relief.
- Particularly beneficial for tumors with intermediate or poor response to chemotherapy or RT (e.g., NSCLC, malignant pleural mesothelioma).
- Recommended for recurrent SVC Syndrome cases.
i) For Chemosensitive Malignancies (e.g., SCLC, NHL, Germ Cell Tumors, Breast Cancer)
- Systemic chemotherapy is preferred over RT or endovascular stenting (Grade 2C).
ii) Newly Diagnosed NSCLC
- Endovascular stent placement is preferred over initial chemotherapy for symptom relief (Grade 2C).
- Post-stent therapy:
- RT (alone or in combination) is suggested for treating mediastinal disease (Grade 2C).
iii) Surgical Resection with SVC Reconstruction
- Considered as part of a multimodal treatment approach for selected cases of thymoma, thymic carcinoma, and residual mediastinal germ cell tumors after chemotherapy.
References
- UpToDate.com
- Respiratory Care, May 2011, 56(5): 653-666