1. Overview of Esophageal Candidiasis
1) Candida Species and Pathophysiology
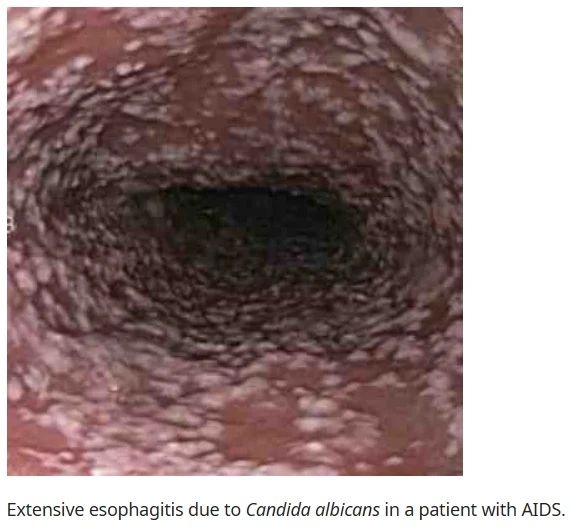
Candida species are yeast organisms that colonize the epithelial surfaces of the gastrointestinal and genitourinary tracts.
- Normally, Candida species exist as commensals in the esophagus, but when host defense mechanisms are compromised, they proliferate and form adherent plaques.
- Local or systemic immune dysfunction can lead to excessive Candida growth and subsequent infection.
2) Common Pathogens
The most common Candida species causing esophageal candidiasis are:
- C. albicans
- C. glabrata
- C. tropicalis
3) Risk Factors
Esophageal candidiasis is one of the most common opportunistic infections. It occurs in individuals with the following conditions:
- Immunosuppression
- Inappropriate use of antibiotics and hormones
- Endocrine disorders
- Nutritional deficiencies
- Chemotherapy and radiation therapy
- Malignancies
i) Underlying Diseases
- HIV/AIDS: Approximately 10% of HIV patients develop esophageal candidiasis in their lifetime.
- Diabetes mellitus, peptic ulcer disease, and post-transplant patients on immunosuppressants
- Achalasia and esophageal stasis
ii) Use of Proton Pump Inhibitors (PPI)
- PPIs are the most common cause of esophageal candidiasis in immunocompetent individuals.
iii) Smoking
- The presence of chemical substances in tobacco weakens the local immune defense of the esophageal squamous epithelium.
- This facilitates the invasion and proliferation of commensal Candida species such as Candida albicans, leading to esophageal candidiasis.
2. Clinical Features and Diagnosis of Esophageal Candidiasis
1) Clinical Symptoms
The most common symptoms of esophageal candidiasis include:
- Odynophagia
- Dysphagia
- Retrosternal pain
- Other symptoms: abdominal pain, heartburn, weight loss, diarrhea, nausea, vomiting, and melena
2) Diagnosis
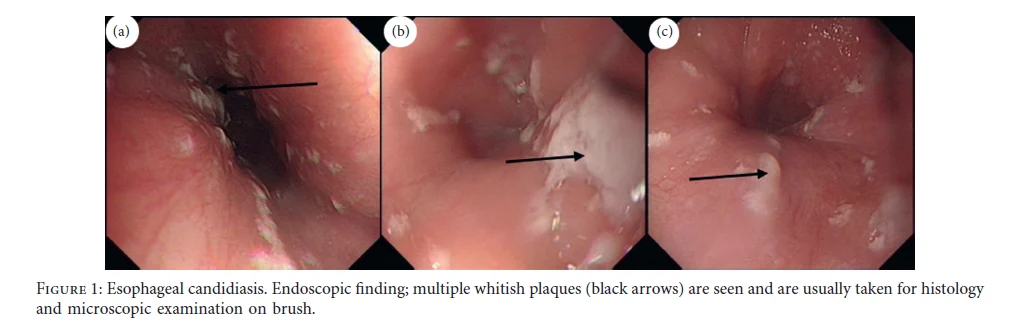
i) Endoscopic Examination
- Direct visualization of the esophagus confirms the diagnosis.
- White plaques on the esophageal mucosa or adherent exudates that cannot be easily removed indicate infection.
ii) Histopathological Examination
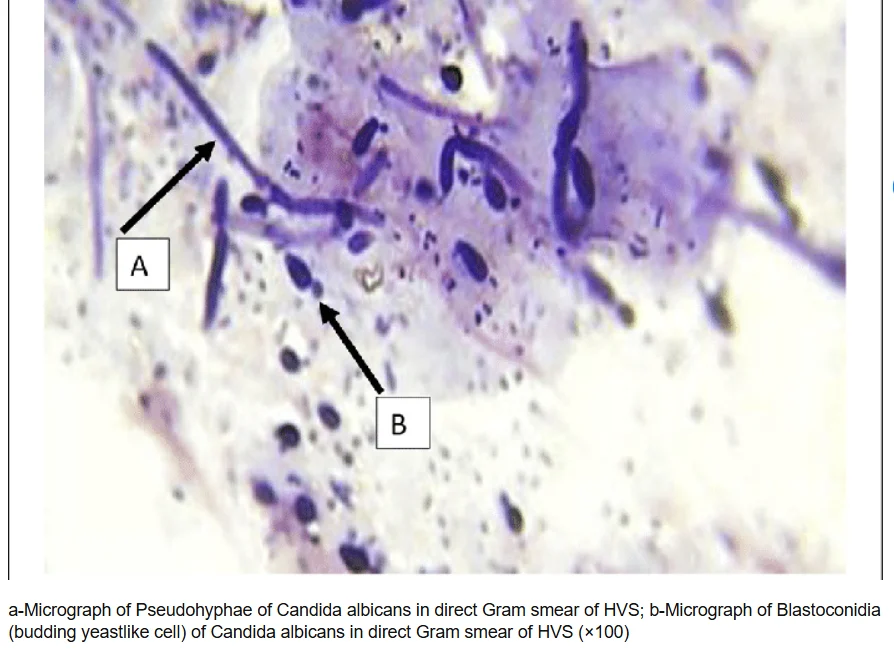
- Hematoxylin and eosin (H&E) staining is used to confirm Candida infection.
- Candida species typically appear as pseudohyphae.
iii) Barium Swallow Study
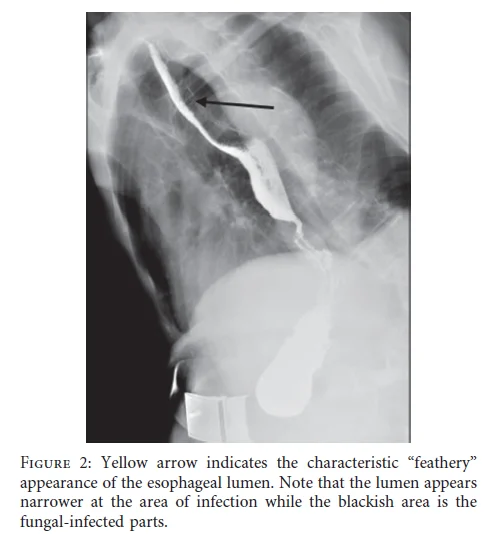
- Abnormal esophageal peristalsis in the upper and lower esophagus may be observed.
- In advanced stages, strictures may be detected as an alternative to endoscopy.
iv) Differential Diagnosis
Esophageal candidiasis must be distinguished from:
- Cytomegalovirus esophagitis
- Herpes simplex virus esophagitis
- Eosinophilic esophagitis
- Pill-induced esophagitis
- Gastroesophageal reflux disease
- Radiation-induced esophagitis
3. Treatment and Prognosis of Esophageal Candidiasis
1) Treatment
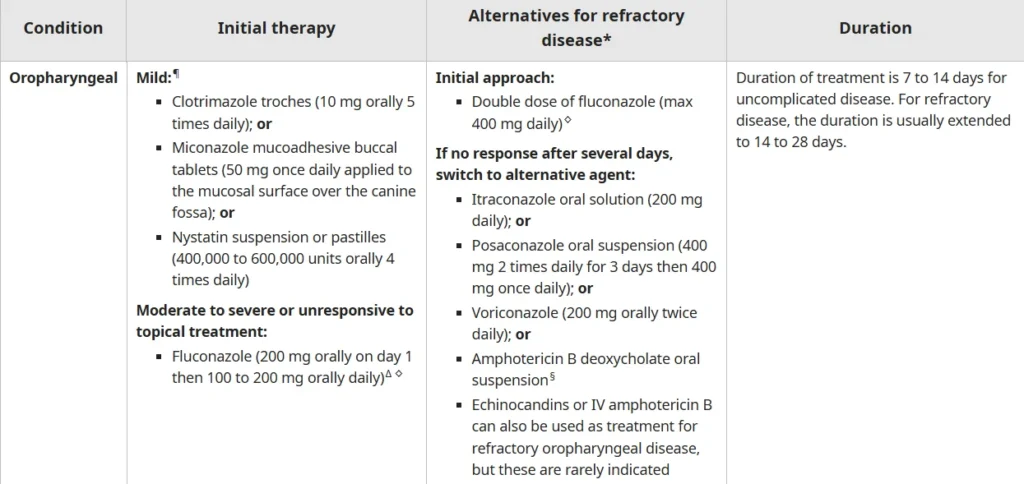

- Systemic antifungal therapy is required.
- Typical duration of treatment: 14-21 days
- For severe cases or those unable to take oral medications, intravenous therapy is recommended.
i) First-line therapy
- Fluconazole: 400 mg IV or PO on the first day, followed by 200-400 mg daily
ii) Treatment for Fluconazole-Resistant C. glabrata
- Echinocandin therapy is preferred.
- If fluconazole resistance is confirmed, the dosage may be increased to 800 mg per day.
2) Prognosis and Complications
- Most cases respond successfully to antifungal therapy.
- Potential complications:
- Necrotizing esophageal candidiasis
- Esophageal stricture
Reference : uptodate.com, Canadian Journal of Gastroenterology and Hepatology Volume 2019,
Article ID 3585136, 6 pages.