1. Myelodysplastic Syndromes (MDS)
① Definition and Characteristics
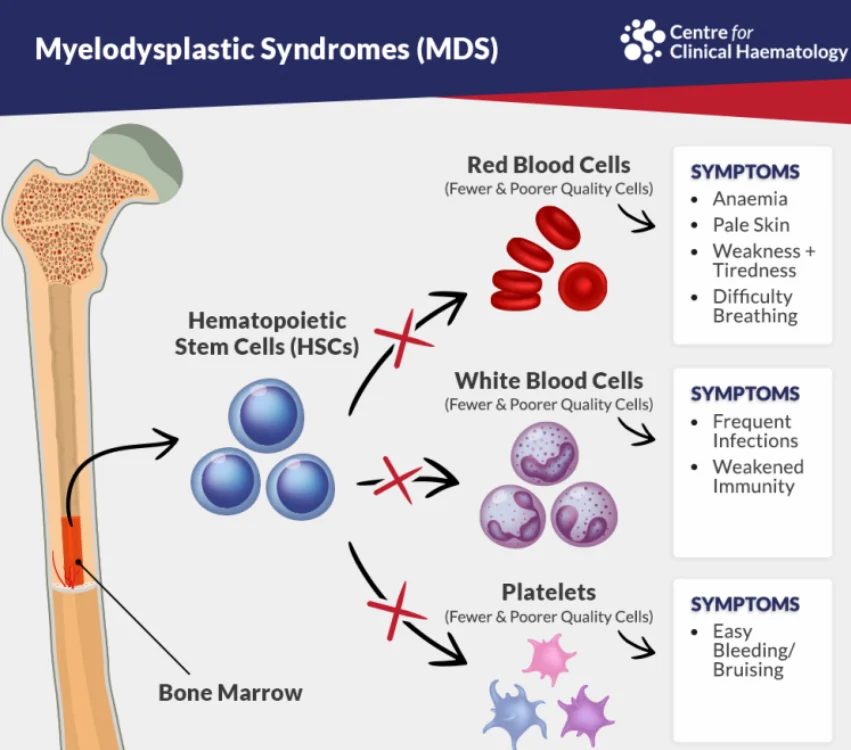
- Myelodysplastic syndromes (MDS) refer to a group of hematologic malignancies characterized by dysplastic cell maturation and isolated or multiple cytopenias (anemia, neutropenia, thrombocytopenia)
- MDS shares clinical and pathological features with acute myeloid leukemia (AML), but the proportion of blasts in peripheral blood and bone marrow is lower in MDS (<20% by definition)
- As a result, patients with MDS are at risk for symptomatic anemia, infections, bleeding, varying degrees of bone marrow failure, and progression to AML
- The majority of morbidity and mortality in MDS is due to complications from cytopenias rather than transformation to AML
2. Hematologic Complications of Myelodysplastic Syndromes (MDS)
① Evaluation of Anemia
- More than 75% of MDS patients develop anemia, with half having hemoglobin (Hb) levels below 10 g/dL.
- Anemia may present with symptoms such as fatigue, anorexia, weight loss, angina, dizziness, dyspnea, headache, and cognitive impairment.
- Causes of anemia should be evaluated, including blood loss, hemolysis, renal failure, medications, nutritional deficiencies, thyroid dysfunction, autoimmune diseases, and anemia of chronic disease.
- Diagnostic workup includes:
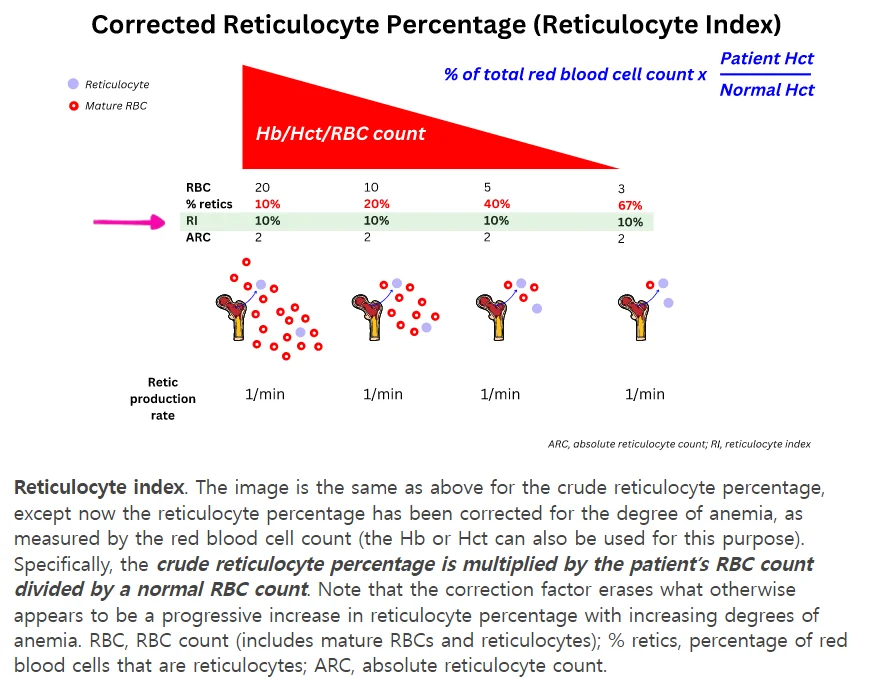
- Complete blood count (CBC), peripheral blood smear, reticulocyte count, and reticulocyte production index (RPI) calculation.
- Evaluation of renal and thyroid function, serum iron, transferrin, ferritin, folate, vitamin B12, copper, and erythropoietin (EPO) levels.
② Treatment of Anemia
For symptomatic patients, treatment is based on MDS risk category, RBC production level (RPI), and serum EPO levels.
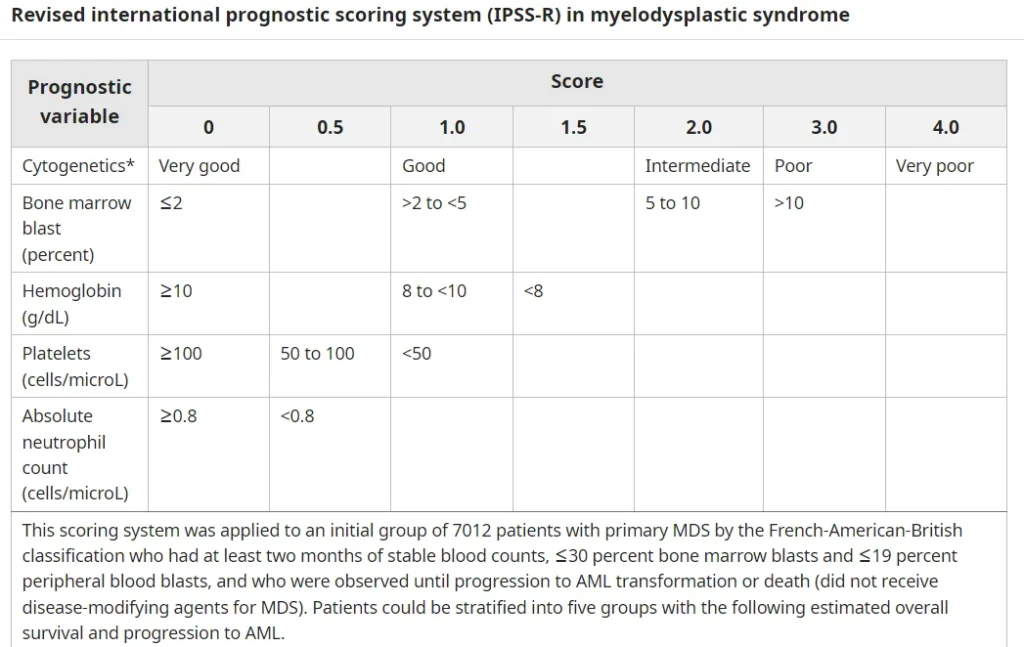
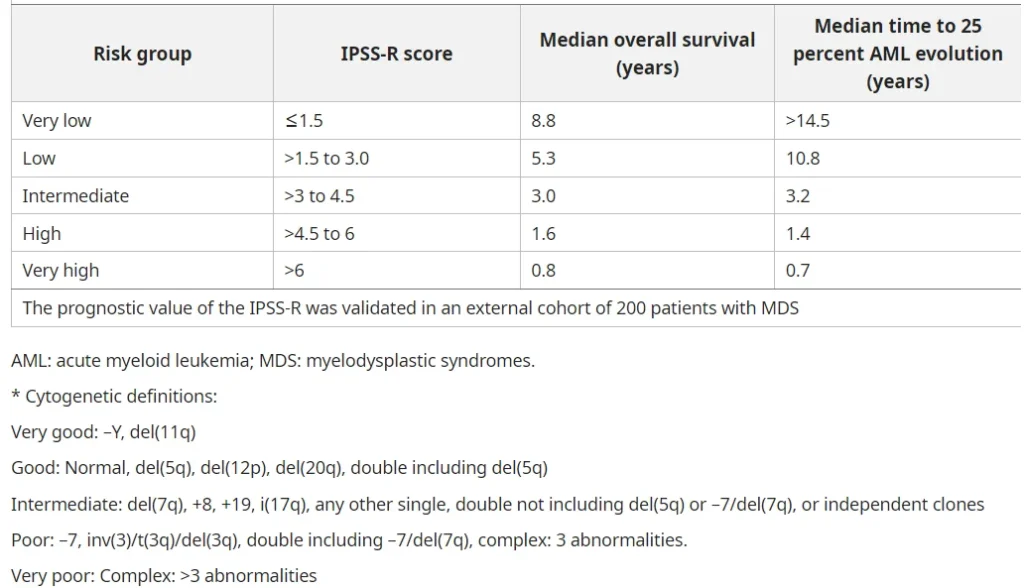
- Low/very low/intermediate risk MDS (IPSS-R ≤4.5 points)
- If RPI <2 and serum EPO ≤500 mU/mL → Initial treatment with erythropoiesis-stimulating agents (ESAs) is recommended.
- If RPI ≥2 or serum EPO >500 mU/mL → RBC transfusion or ESA with/without myeloid growth factors may be considered.
- High/very high-risk MDS (IPSS-R >4.5 points)
- Chronic transfusion therapy alongside definitive treatment of the underlying disease is suggested.
- Correction of contributing factors (e.g., bleeding, hemolysis) is necessary.
- During transfusion, leukoreduced blood products are recommended to reduce the risk of alloimmunization, febrile transfusion reactions, cytomegalovirus (CMV) and other viral infections, and immunosuppression.
③ Infection
- Infection is a major cause of morbidity and mortality in MDS patients.
- Increased infection risk is associated with neutropenia and granulocyte dysfunction.
- Bacterial infections, particularly those involving the skin, are common.
- Neutropenic patients (absolute neutrophil count <500/microL) require urgent evaluation, blood cultures, and immediate empiric antibiotic therapy.

④ Bleeding
- Bleeding in MDS may result from thrombocytopenia, qualitative platelet dysfunction, or coagulation disorders.
- Platelet transfusion recommendations:
- Prophylactic transfusion for asymptomatic patients with platelet counts <10,000/microL
- Higher threshold for patients with active bleeding, fever, severe infection, pulmonary dysfunction, coagulopathy, or CNS abnormalities.

Reference: UpToDate.com