1. Hypoxic-Ischemic Brain Injury (HIBI)
Brain Physiology and Anatomy
- The brain constitutes only 2% of body weight but accounts for 20% of total oxygen consumption.
- Inadequate cerebral blood circulation ultimately leads to neuronal cell death.
Increased Intracranial Pressure (ICP)
- Cerebral ischemia can directly cause ICP elevation.
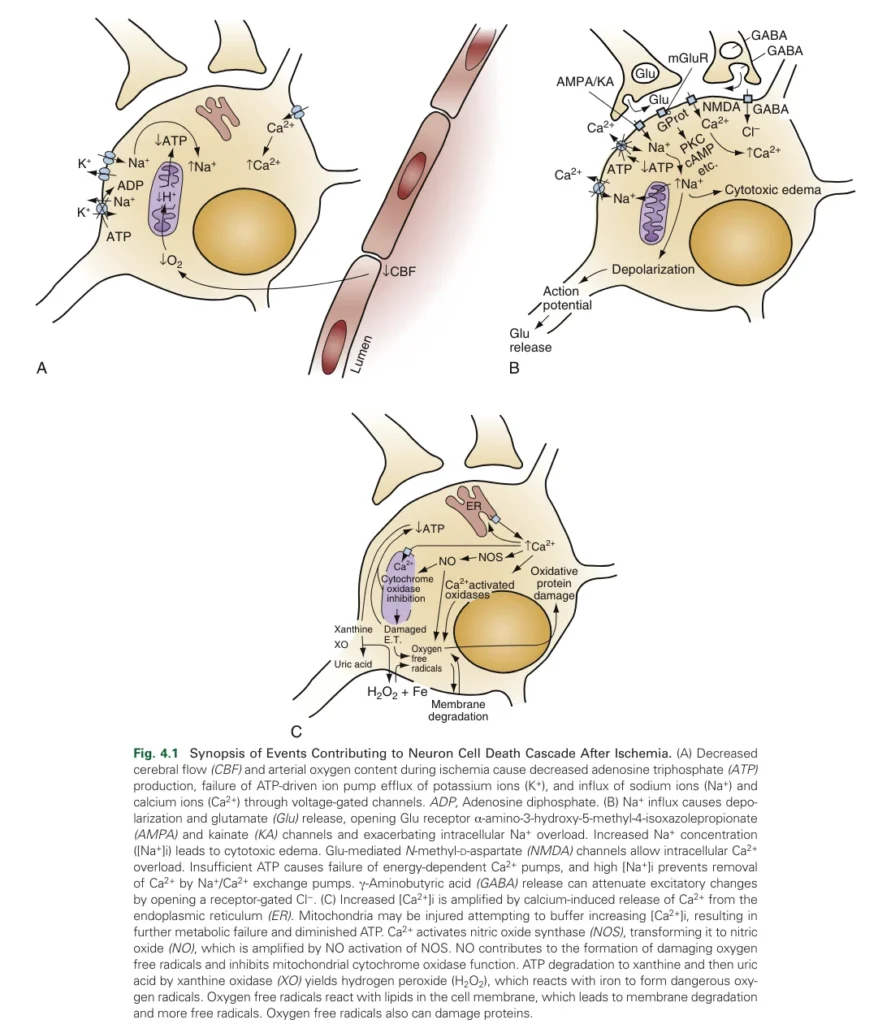
- Failure of oxidative phosphorylation leads to ATP depletion, making it impossible to actively maintain the osmotic gradient.
- Increased intracellular osmotic pressure results in water influx and cytotoxic edema.
- Peak swelling occurs within 48-72 hours post-injury.
2. Management of Hypoxic-Ischemic Brain Injury
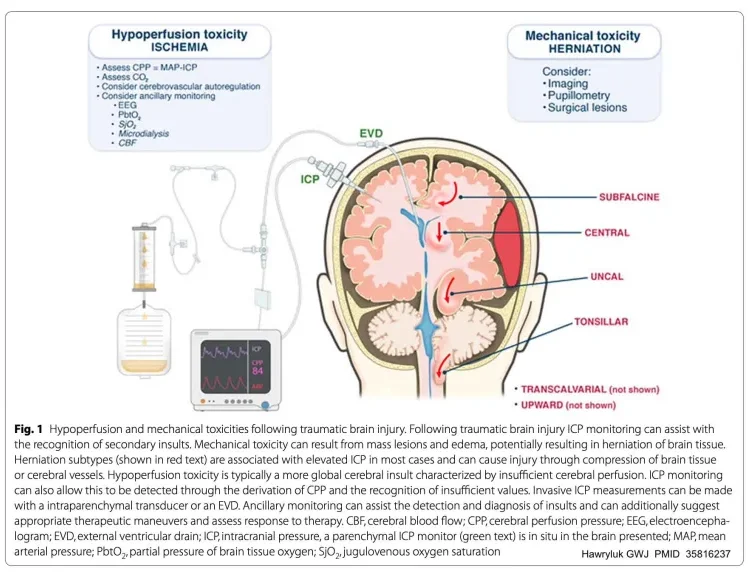
ICP Management
ICP should be managed immediately if it exceeds 22 mmHg to prevent poor neurological outcomes.
i) Pain and Fever Control
- All patients with traumatic brain injury at risk of ICP elevation require pain and fever management.
- Pain control: Fentanyl, a hemodynamically stable opioid, is recommended (25-50 mcg every 5 minutes as needed).
- Fever management:
- Increased body temperature raises cerebral metabolic demand by 8-13% per 1°C.
- Enhances glutamate release, oxidative free radical production, cytoskeletal damage, and blood-brain barrier disruption, leading to vasogenic edema.
ii) Adequate Sedation
- Avoid coughing or ventilator dyssynchrony.
- Propofol: Reduces cerebral metabolic activity, oxygen demand, and blood flow. However, it may cause hypotension, necessitating vasopressor support.
- Dexmedetomidine: Helps control patient agitation, facilitates ET tube adaptation, and allows frequent neurological exams but does not suppress respiratory drive, increasing the risk of ventilator dyssynchrony.
iii) Management of Acute ICP Elevation or Herniation Syndrome
- Hyperosmolar therapy (Mannitol or Hypertonic Saline):
- Works by drawing water across the blood-brain barrier to reduce ICP.
- Mannitol: 0.25-1g/kg every 6 hours until serum osmolality reaches 320 mOsm/kg. Preferred in fluid overload conditions.
- 23.4% Hypertonic Saline: 30-60 mL every 6 hours, with a serum sodium target of 160 mEq/L. Central venous administration recommended for safe delivery.
- 3% Hypertonic Saline: Can be continuously infused at 30-50 mL/hour.
iv) ICP Management Protocol
- Elevate the head of the bed to 30°.
- Maintain a neutral position for the neck and head to avoid jugular venous compression.
- Treat fever with antipyretics and surface cooling to maintain a temperature below 37°C.
- Minimize ICP triggers such as frequent repositioning and suctioning.
- Avoid supine positioning as much as possible.
- Initiate hyperosmolar therapy as needed.
Seizure Management
- Seizures: Can increase cerebral metabolism by 300-400%, exacerbating oxygen supply-demand mismatch, leading to metabolic failure and neuronal damage.
- Prolonged post-cardiac arrest seizures and status epilepticus are associated with poor neurological outcomes.
- Continuous EEG monitoring is recommended.
- Routine prophylactic anticonvulsants are not recommended.
- Lorazepam: First-line agent, 0.1 mg/kg (max 4 mg).
- Second-line IV loading options:
- Levetiracetam: 60 mg/kg (max 4500 mg)
- Valproic acid: 40 mg/kg (max 3000 mg)
Optimization of Perfusion and Oxygen Delivery
i) Hypotension Management
- Low cerebral blood flow (CBF) contributes to poor outcomes.
- For post-cardiac arrest patients, recommended BP targets:
- MAP ≥65 mmHg
- SBP ≥90 mmHg
- Rapid correction of low arterial pressure with intravascular volume expansion and vasopressors is essential.
- Target SBP <140 mmHg, using antihypertensives if needed.
ii) Carbon Dioxide Regulation
- CO₂ is a potent cerebrovascular modulator.
- Hyperventilation-induced hypocapnia:
- Lowers arterial CO₂ (PaCO₂), causing rapid CBF reduction (2% decrease in CBF per 1 mmHg PaCO₂ drop).
- Temporarily reduces ICP by decreasing total cerebral blood volume.
- May delay brainstem herniation but also causes cerebral ischemia due to excessive vasoconstriction and increased cerebrovascular resistance (CVR).
- Use of hyperventilation should be limited to refractory herniation not responding to osmotic therapy.
- Maintain PaCO₂ between 35-40 mmHg to balance safety and effectiveness.
iii) Oxygenation Management
- Use the lowest possible FiO₂ to maintain PaO₂ 80-120 mmHg and SpO₂ >90%.
Surgical Intervention
- Decompressive craniectomy and hematoma evacuation should be considered in cases where medical ICP management fails.
Targeted Temperature Management (TTM)
- Neuroprotective mechanisms of hypothermia:
- Reduces glutamate release, metabolic demand, free radical formation, and inflammatory cytokine production.
- Mild hypothermia (32-34°C) provides neuroprotection with fewer side effects compared to more profound hypothermia.

Reference: Rosen’s Emergency Medicine, 10th Edition.