1. Pertussis
① Overview of Pertussis
- Pertussis is a highly contagious acute respiratory disease caused by Bordetella pertussis.
- Bordetella pertussis
- A gram-negative coccobacillus.
- Survives only a few hours in respiratory secretions outside the human body.
② Epidemiology
- Despite widespread vaccination, the incidence of pertussis has increased since the 1990s, with peaks occurring every 3–5 years.
③ Transmission
- Pertussis is transmitted via respiratory droplets.
- It spreads through coughing, sneezing, or prolonged close contact in shared airspace.
④ Complications
- Most common complications in infants:
- Apnea, pneumonia, weight loss due to post-tussive vomiting and feeding difficulties
- Other complications include:
- Seizures, encephalopathy, death, sleep disturbances, pneumothorax, epistaxis, subconjunctival hemorrhage, subdural hematoma, rectal prolapse, urinary incontinence, rib fractures
2. Clinical Features and Diagnosis
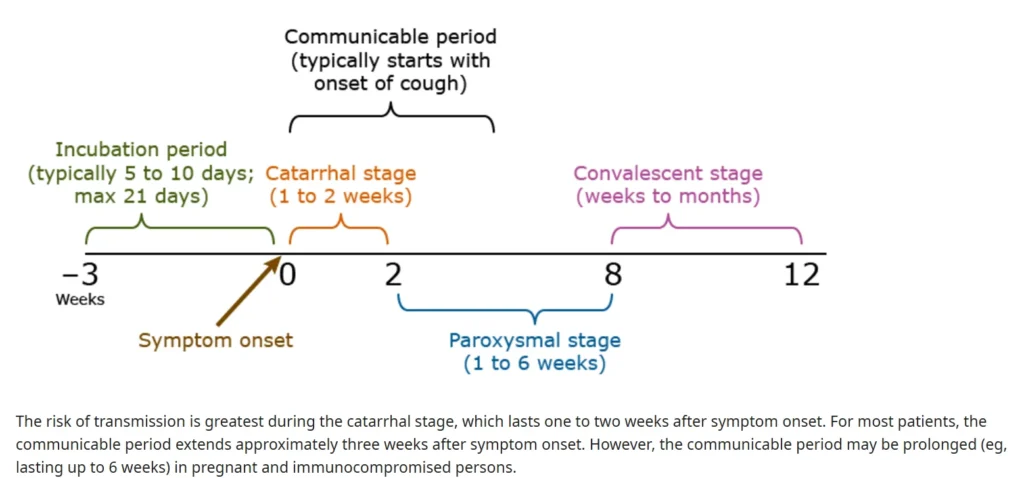
① Clinical Features
The “100-day cough” progresses in three stages:
i) Catarrhal Stage
- Resembles a viral upper respiratory tract infection with mild cough and rhinorrhea.
- Fever is uncommon.
Lasts 1–2 weeks.
ii) Paroxysmal Stage
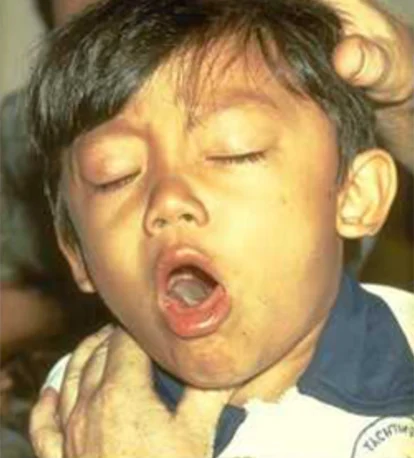
- Severe coughing fits (paroxysms) develop.
- Children may gag, appear lethargic, and struggle to breathe. Symptoms are worse at night.
- “Whoop”—a high-pitched inspiratory sound—may follow coughing fits.
Lasts 2–8 weeks. - iii) Convalescent Stage
- Cough gradually resolves over weeks to months.
- Intermittent coughing may recur with subsequent upper respiratory infections.
② Laboratory Findings
- Nonspecific findings:
- Lymphocytosis
- WBC count may be normal
③ Radiologic Findings
- Nonspecific chest X-ray findings:
- Normal
- Perihilar infiltrates or atelectasis
④ Diagnosis
i) Infants <4 months
- Persistent cough, rhinorrhea, apnea, seizures, cyanosis, vomiting, failure to thrive
- Lymphocytosis (WBC ≥20,000 cells/microL, lymphocytes ≥50%)
- Pneumonia
- History of exposure to a person with prolonged cough
ii) Children >4 months
- Paroxysmal dry cough lasting ≥7 days
- Cough with rhinorrhea, whoop, apnea, post-tussive vomiting, conjunctival hemorrhage, or sleep disturbance
- Sweating between coughing fits
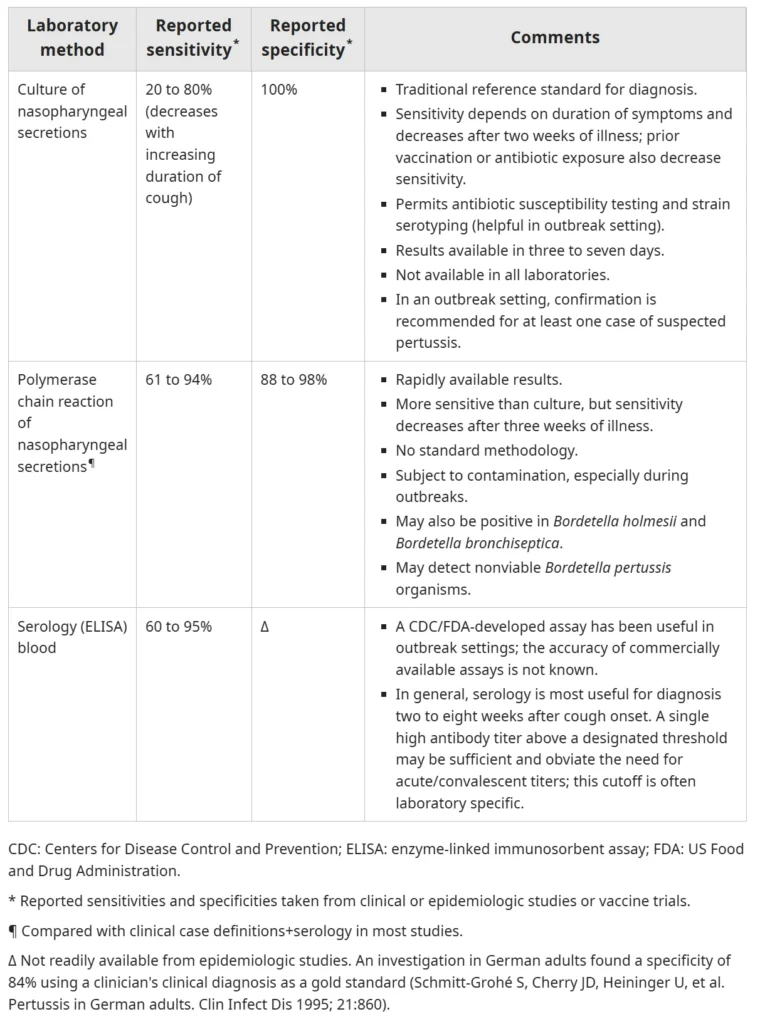
iii) Diagnostic Tests
- Clinical diagnosis: Cough ≥2 weeks with paroxysms, whoop, or post-tussive vomiting.
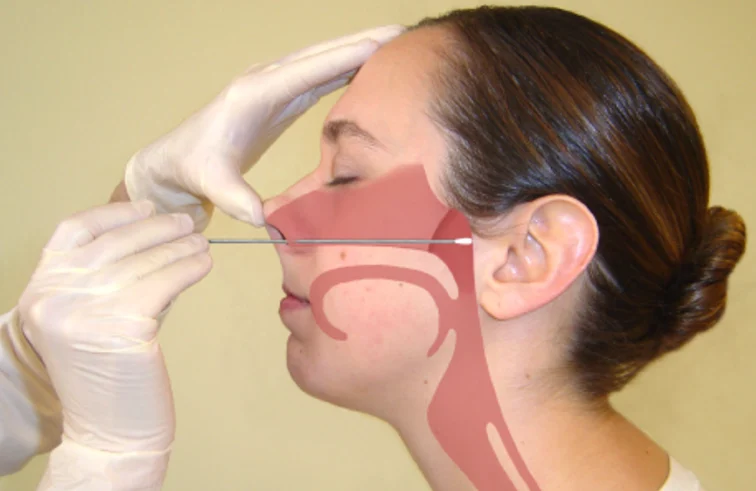
- Confirmatory tests: Bacterial culture, PCR, or serology using nasopharyngeal swabs or aspirates.
3. Treatment and Prevention
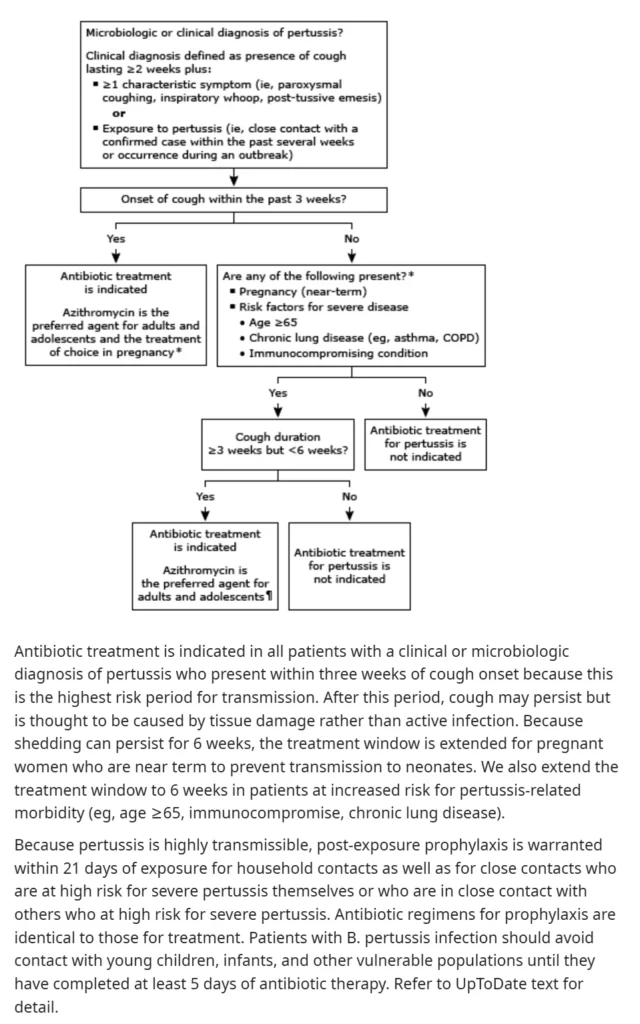
① Antibiotic Therapy
- Recommended within 3 weeks of cough onset to reduce transmission.
- After 3 weeks, antibiotics are not routinely given.
- CDC-recommended regimens:
- Azithromycin: 500mg PO on day 1, then 250mg PO daily for days 2–5.
- Clarithromycin: 500mg PO twice daily for 7 days.
- TMP-SMX if macrolides are contraindicated.
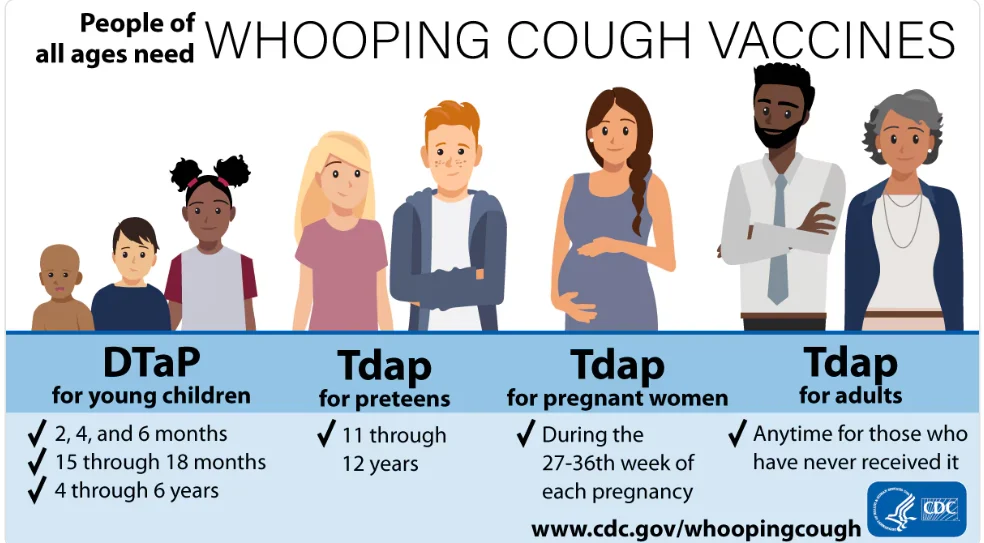
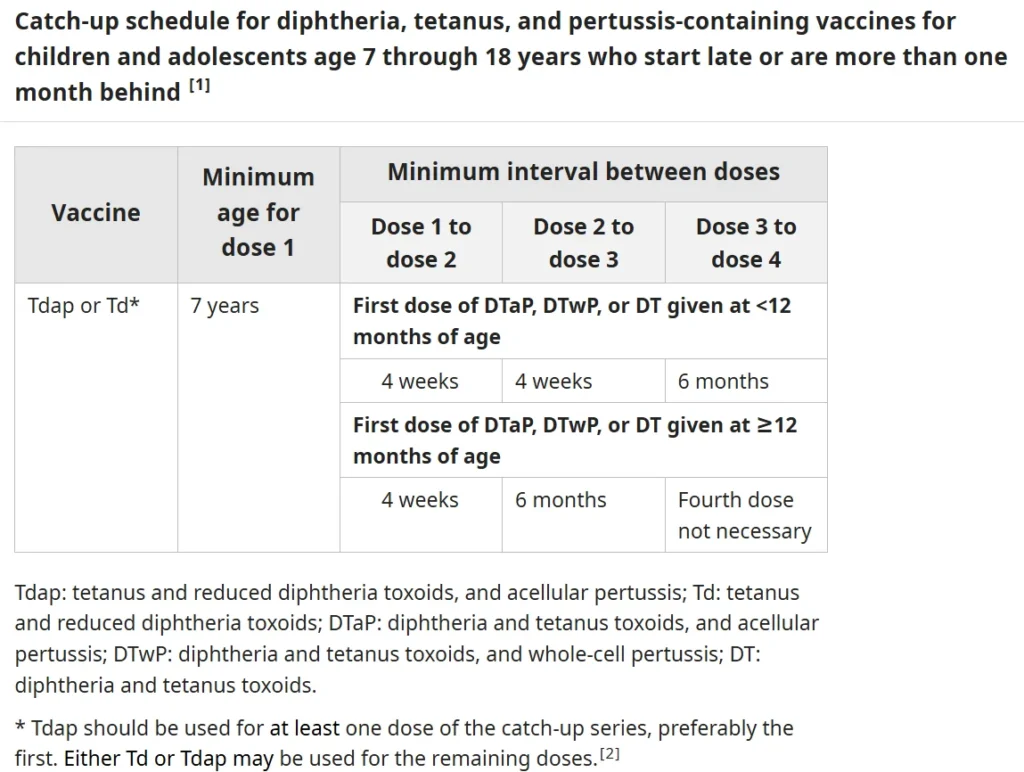
② Vaccination
- Tdap booster recommended for adolescents (11–18 years) and adults every 10 years.
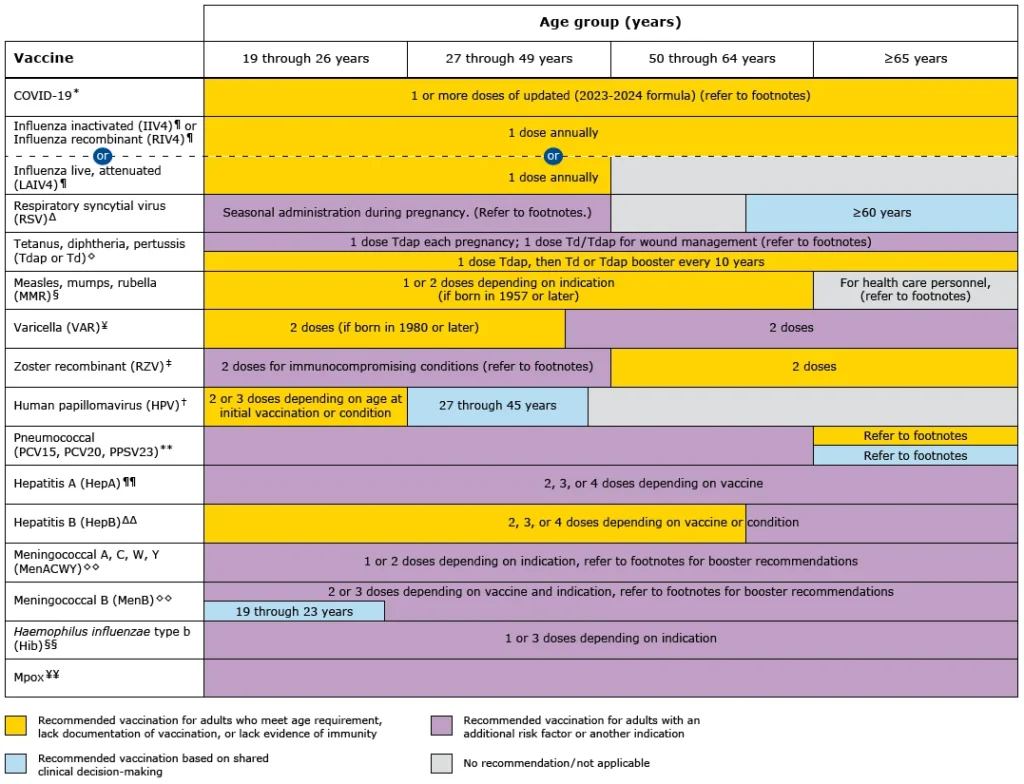
Reference: UpToDate.com