1. Criteria for Severe Trauma

1) Vital Signs
- Oxygen saturation < 90%
- Systolic blood pressure < 90 mmHg
- Respiratory rate: <9 or >29 breaths/min
- Glasgow Coma Scale (GCS) score < 14
2) Mechanism of Injury
- Penetrating injury to the head, neck, chest, abdomen, or pelvis
- All gunshot wounds
- Open or depressed skull fractures, pelvic fractures, multiple proximal long bone fractures, flail chest
- Amputation
- Blast or crush injury
3) Burns
- Adults: >15% total body surface area (TBSA); Pediatric or elderly: >10% TBSA
- Airway burns
- Combination of trauma and burns
4) Traffic Accidents
- High-speed collision (>30 mph = ~48 km/h) or pedestrian struck at >20 mph (~32 km/h)
- Ejection from a motorcycle or vehicle
- Vehicle rollover
- Passenger fatality
- Extrication time > 20 minutes
5) Falls
- Height >3 meters
6) Drowning or Submersion Accidents
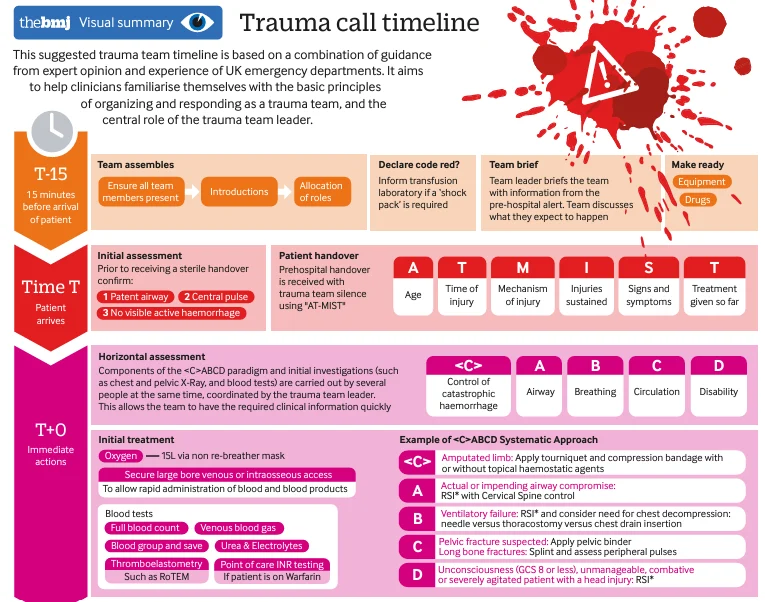
2. Initial Evaluation upon Arrival
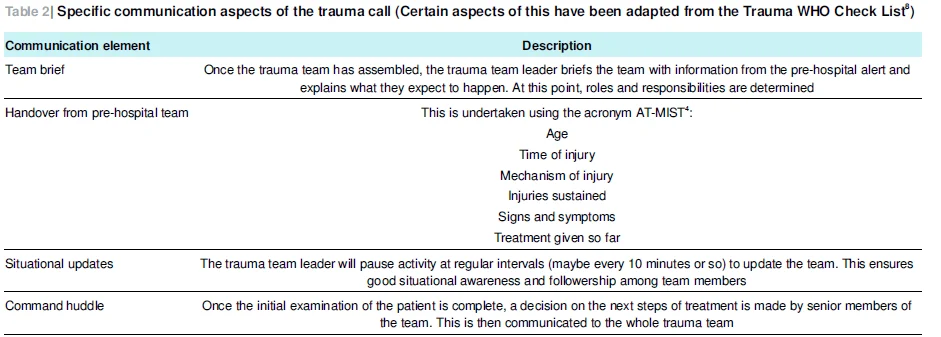
1) Handover Information
- Age, time of injury, mechanism of injury, ongoing injuries, symptoms and signs, treatments given
- If airway intervention or ongoing hemorrhage is needed, emergency treatment should precede handover
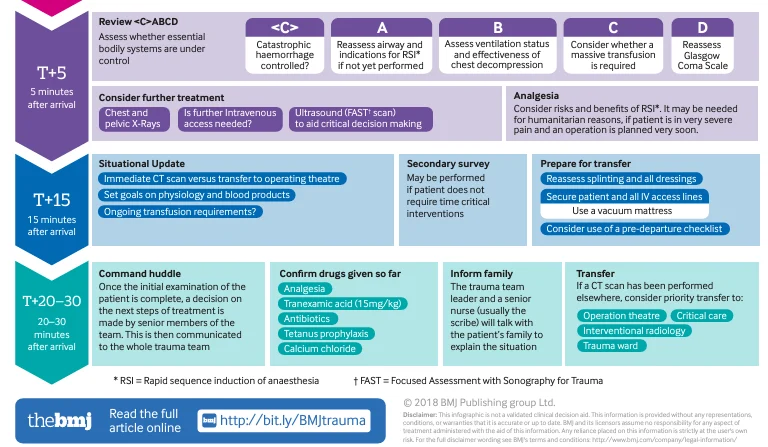
2) T+0 (Immediate)
- Primary Survey
- C (Control of catastrophic hemorrhage): Apply pressure bandage or tourniquet for hemorrhage control
- A (Airway): Maintain and secure airway
- B (Breathing): Assess for tension pneumothorax; consider needle thoracostomy or chest drain insertion if needed
- C (Circulation): Apply pelvic binder for suspected pelvic fracture; splint for femur fractures, check peripheral pulse
- D (Disability): Assess consciousness level
- Establish large-bore IV access for rapid fluid resuscitation and blood transfusion, provide oxygen
3) T+5 (5 Minutes Post-Arrival)
- Reassess ABCD: Hemorrhage control, airway patency, adequate ventilation, need for massive transfusion, and consciousness level
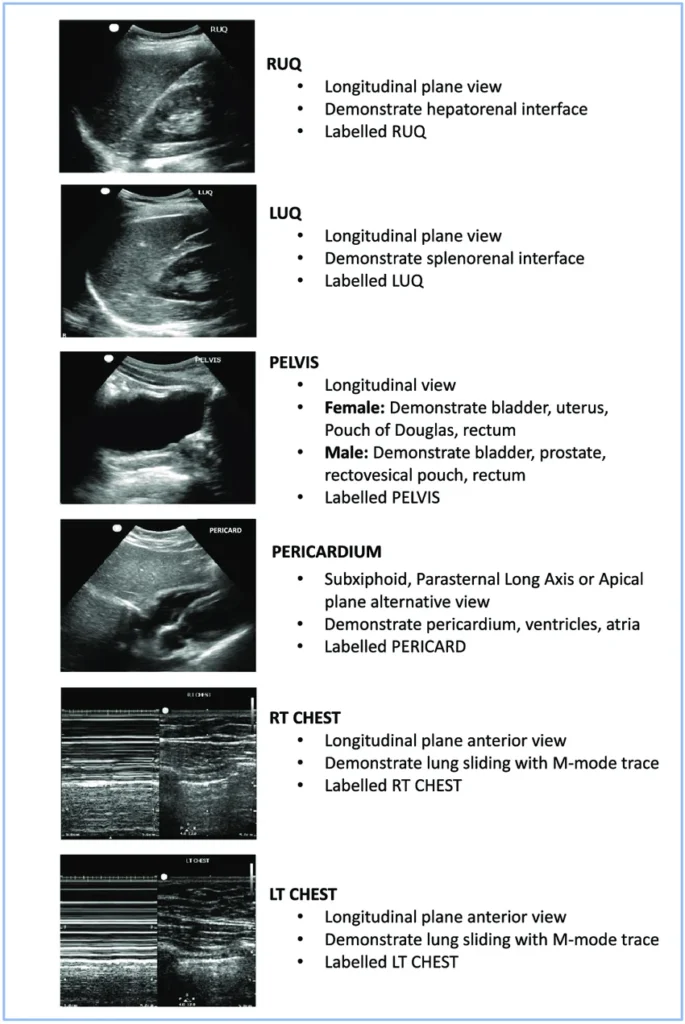
- Consider additional diagnostics: Chest & pelvic X-ray, IV access evaluation, FAST scan
4) T+15 (15 Minutes Post-Arrival)
- Decide on immediate CT scan vs. transfer to operating room
- Assess need for ongoing transfusion
5) T+20-30 (20-30 Minutes Post-Arrival)
- Review initial assessment and determine next treatment steps with the team
- Inform the family about the patient’s condition
3. Considerations for Hemorrhage & Transfusion
1) Hemorrhage Management
- Blood loss up to 30% of total blood volume: May cause mild tachycardia and decreased pulse pressure; if undetected early, can lead to shock
- Two 18G or larger IV lines, administer lactated Ringer’s and collect blood samples
- If peripheral IV access is difficult, consider central venous catheterization via subclavian, internal jugular, or femoral vein
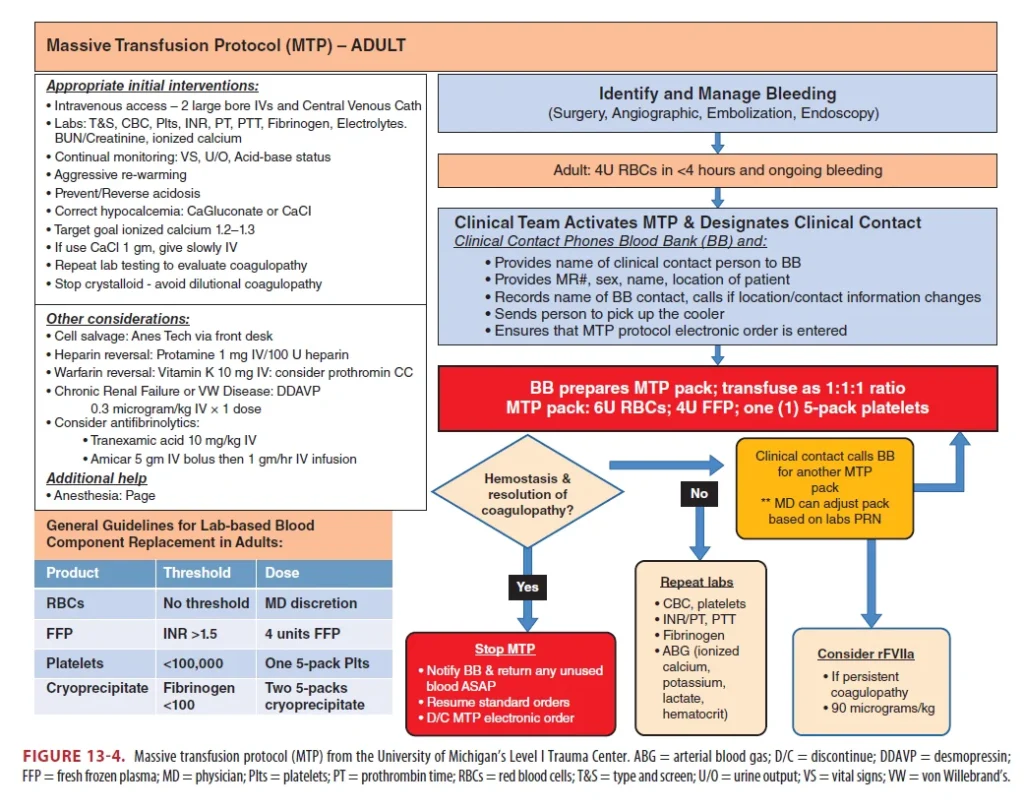
- Massive transfusion protocol (MTP) is needed when >10 units of PRBCs are required in the first 24 hours
- Balanced transfusion (FFP:PLT:PRBC = 1:1:1) is recommended, though the optimal ratio remains uncertain
2) Tranexamic Acid
- Antifibrinolytic agent reducing surgical and trauma-related blood loss
- Blocks plasmin cleavage and fibrin degradation
- Most effective within 1 hour post-injury; administration after 3 hours may be harmful
- Dosage: 1g IV bolus over 10 min, followed by 1g IV every 8 hours
3) Calcium
- Citrate in PRBCs and FFP can cause life-threatening hypocalcemia
- Maintain ionized calcium >0.9 mmol/L
Reference: BMJ 2018;361:k2272, Tintinalli’s Emergency Medicine 9th Edition