1. Transient Tachypnea of the Newborn
① Pathophysiology
Transient tachypnea of the newborn (TTN) is a parenchymal lung disorder characterized by pulmonary edema due to delayed resorption and clearance of fetal alveolar fluid
- TTN is the most common cause of respiratory distress in late preterm and term neonates
- The normal clearance process of fetal alveolar fluid begins before term, continues during labor, and persists after birth
- Approximately 100 mL of fetal lung fluid is removed from the lungs from the onset of labor until birth
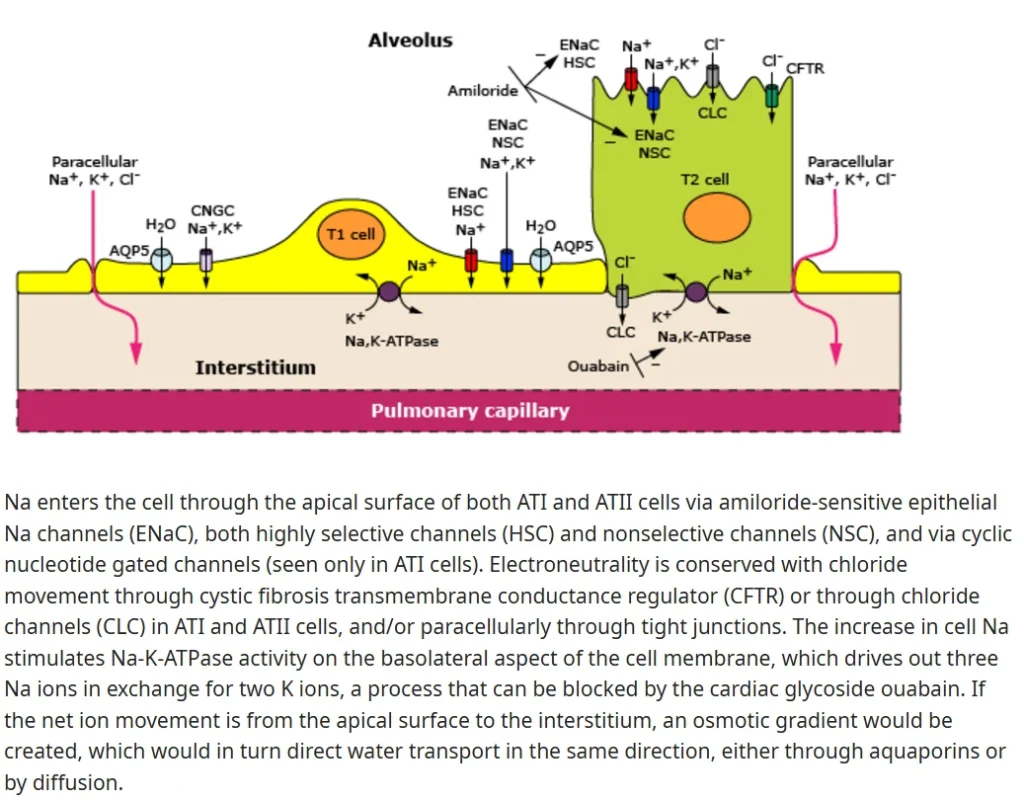
- Increased oxygen tension at birth upregulates epithelial sodium channel (ENaC) gene expression, enhancing sodium and water absorption. However, immature lungs exhibit reduced ENaC gene expression, preventing the transition from secretion to absorption
- Glucocorticoids upregulate ENaC gene expression, facilitating active absorption through sodium channels
② Risk Factors
- Maternal risk factors: Delivery before 39 weeks of gestation, cesarean delivery, gestational diabetes, maternal asthma
- Fetal risk factors: Male sex, perinatal asphyxia, prematurity, small or large for gestational age
- Incidence: Inversely proportional to gestational age. Approximately 10% of neonates born at 33–34 weeks, 5% at 35–36 weeks, and 1% at term develop TTN
2. Clinical Features and Diagnosis
① Clinical Features
- Onset of TTN: Typically begins at birth or within the first 2 hours of life
- Most prominent symptom: Tachypnea (>60 breaths per minute)
- Severe cases: Cyanosis, increased work of breathing, nasal flaring, mild intercostal and subcostal retractions, expiratory grunting
- Duration: Mild-to-moderate TTN resolves within 12–24 hours, while severe cases may persist up to 72 hours
② Diagnosis
- Clinical diagnosis: Based on early-onset respiratory distress and characteristic chest imaging findings
- Confirmation: Symptoms resolve within 12–24 hours
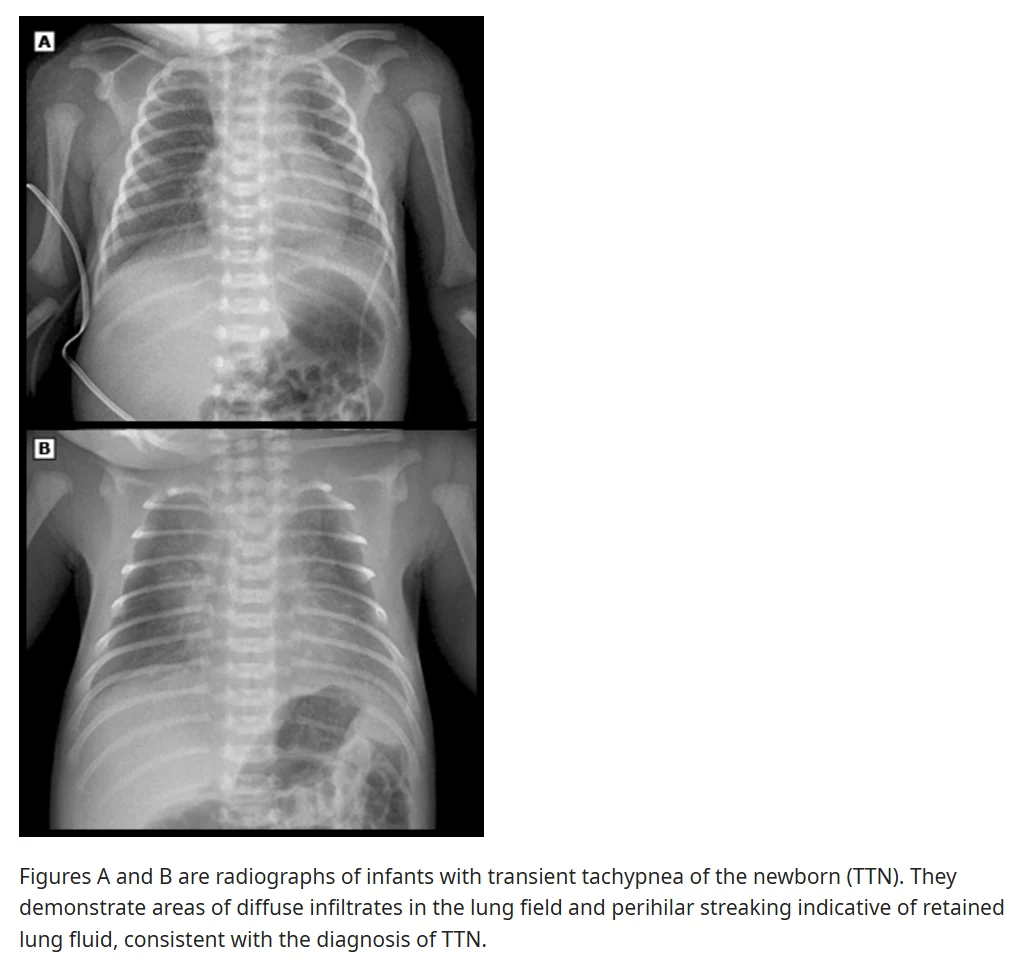
- Chest radiographic findings
- Increased lung volumes with flattened diaphragms
- Mild cardiomegaly
- Prominent vascular markings around the hilum, “sunburst pattern”
3. Treatment
Supportive and Conservative Management
(Because TTN is a self-limited and benign condition) (∵ Self-limited condition, Benign)
① Maintain a neutral thermal environment
② Nutrition
- If respiratory rate exceeds 60–80 breaths per minute or increased work of breathing is present, oral feeding is not possible
- Provide nasogastric feeding or intravenous fluids as needed
③ Oxygen Therapy
- Adjust oxygen supplementation to maintain SpO2 at 90–95%
- TTN neonates rarely require FiO2 > 0.4
④ Fluid Restriction
⑤ Avoid diuretic therapy
⑥ Prognosis
Reference
uptodate.com., NIH-Transient Tachypnea of the Newborn Kanishk Jha